A group calling themselves Take The Flour Back are opposed to Genetically Modified wheat. Their plan is to visit Rothamsted Park on the 27th of May 2012 and destroy the GM crops being grown as part of the experiment described here:
“Scientists from Rothamsted Research are conducting a controlled experiment to test wheat, genetically modified to repel greenfly and blackfly, which could help reduce pesticide use and promote sustainable agriculture in the future.”
Scientists from Rothamsted Research recorded this video in an effort to open dialogue with the protesters.
You can read a written message from the scientsts here: Rothamsted Appeal Letter [PDF file]
Misinformation
The protest group make a few assertions in favour of their vandalism:
Rothamsted have planted a new GM wheat trial designed to repel aphids. It contains genes for antibiotic-resistance and an artificial gene ‘most similar to a cow’.
Rothamsted deny that they have used any genetic material from cows. In fact, the odour is produced by a protein called (E)-β-farnesene which is also produced by hundreds of other plants including plants which we consume, such as Hops. Rothamsted state: “To suggest that we have used a ‘cow gene’ and that our wheat is somehow part-cow betrays a misunderstanding which may serve to confuse people or scare them but has no basis in scientific reality.”
There is no market for GM wheat anywhere in the world.
This isn’t true. Plenty of GM products are sold and consumed, although some of that is through abusive behaviour by large US businesses. That is a different problem to address. Perhaps they mean that people are generally opposed to GM food, but whether true or not that should not stop experiments that could have far-reaching benefits. People should be allowed to make their own choice. I fully support the idea that any product sold which contains GM ingredients should be labelled to allow people to choose.
This experiment is tax-payer funded, but Rothamsted hope to sell any patent it generates to an agro-chemical company.
Rothsted completely refute this:
Our work is publically funded, we have pledged that our results will not be patented and will not be
owned by any private company - if our wheat proves to be beneficial we want it to be available to
farmers around the world at minimum cost.
Take The Flour Back continue:
La Via Campesina, the world’s largest organisation of peasant farmers, believe GM is increasing world hunger. They have called for support resisting GM crops, and the control over agriculture that biotech gives to corporations.
I wonder how this organisation can support this statement. I do not believe that GM crops increase world hunger, but I do know that large companies are abusing patents to force the purchase of GM seeds in many cases. This is a problem with those companies and not with GM products.
‘Take the Flour Back’ will be a nice day out in the country, with picnics, music from Seize the Day and a decontamination. It’s for anyone who feels able to publically help remove this threat and those who want to show their support for them.
Wrong. That should read:
Take the Flour Back’ will be a nice day out in the country, with picnics, music from Seize the Day and vandalism and destruction of scientific experiments before the evidence can be gathered by people who fear what they do not understand.
A news story on the Green Party website also added:
The trial is happening in the open air, meaning that when it starts to flower it can cross contaminate other wheat crops and wild grasses. This is a real threat.
However this is false. The wheat used for this experiment is self-pollinating and the flower fertilises itself rather than dispersing pollen through the air to another plant. The seeds are too heavy to disperse in the wind and the plant has no adaptations to facilitate insect pollination. Even so, the researchers have taken precautions against contamination:
The GM plots will be separated from the edge of the trial by 10 meters of barley (or space) plus a 3 metre ‘pollen barrier’ of wheat that helps to contain pollen from the GM plants within the trial site. All these plants are treated as though they are GM and harvested /destroyed at the end of the trial. There will be no cereals grown for 20 metres outside the boundary of the site and no wild relatives of wheat that can cross with our cultivated variety exist in the vicinity.
Couch grass species, distant relatives of wheat will be controlled in a 20 metre wide area around the trial site to avoid any slight possibility of cross-pollination.
The right to protest
I am completely in favour of a right to free speech and the right to protest, even with people that I do not agree with. However, I am horrified at the idea of destroying scientific research. To make good policy we need knowledge, we need evidence. We obtain evidence through research. To destroy this research before we have any results is like setting fire to a library. Risk assessments have been carried out, precautions have been taken, consultations were carried out. Even if those who object did not engage at that time surely if there were a danger then they could attempt to stop things now through legal processes which will make a decision based on evidence. I think the protesters have probably not done so because the evidence is not on their side.
Why I am leaving the Green Party
I have explained why I oppose Take The Flour Back, but I am also resigning my membership of The Green Party over this issue. London Assembly Member and former candidate for London Mayor Jenny Jones tweeted on the 10th of May:
https://twitter.com/GreenJennyJones/status/200465542736396289
This was followed up with a news story on the Green Party website which repeated some of the false statements made by Take The Flour Back and announced that Jenny Jones would attend the protest.
I believe this represents support from the Green Party for vandalism and the destruction of scientific experiments. One of the reasons that I took a long time to join the Green Party after betrayal by the Liberal Democrats in 2010 was the anti-science attitude that I saw with their policies supporting homeopathy and reacting against many things out of fear and contrary to evidence. Indeed, the Green Party knew that this was a problem and recently made an effort to make their policies evidence based. I joined about three months ago when I thought that things had changed but this fiasco over GM experiments has left me feeling that I cannot trust the party. Perhaps I have given the Greens less of a chance than I did the LibDems but after one betrayal I am not waiting around for another.
I no longer feel that I can trust political parties. Manifesto pledges mean nothing. Promises seem to lead to the exact opposite behaviour. Politicians happily lie and mislead the public as to their true intentions. I’ve learnt my lesson. I sent in my resignation to the Green Party a few minutes ago and I will no longer support any political party.
There is a campaign by Sense About Science and a you can sign the petition asking people not to destroy research.
Further Reading
Rothamsted Wheat Trial: Second generation GM technology to emulate natural plant defence mechanisms
I wish to thank my wife and scientific adviser, Karen Sumpter (@missnfranchised)


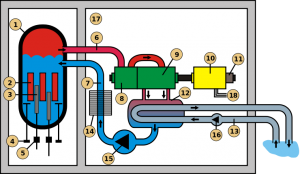
 I will admit, dealing with nuclear waste is a problem. I would like to make some points about this. First of all, fossil fuels also produce waste. That waste in the form of ash, CO2, sulfur dioxide, nitrous oxide and other gasses has traditionally been pumped into the atmosphere where it causes acid rain, smog and climate change. Pollution from fossil fuels affects the workers at the power station and the residents in towns nearby. Recent attempts to scrub pollutants out of smoke before releasing it have reduced this a little, but not enough. Carbon capture will improve things but is very difficult and hugely expensive. Secondly,
I will admit, dealing with nuclear waste is a problem. I would like to make some points about this. First of all, fossil fuels also produce waste. That waste in the form of ash, CO2, sulfur dioxide, nitrous oxide and other gasses has traditionally been pumped into the atmosphere where it causes acid rain, smog and climate change. Pollution from fossil fuels affects the workers at the power station and the residents in towns nearby. Recent attempts to scrub pollutants out of smoke before releasing it have reduced this a little, but not enough. Carbon capture will improve things but is very difficult and hugely expensive. Secondly, 
 I believe many of these methods mentioned here to be a fraud or at most a misplaced faith in something which doesn’t actually have any scientific reason behind it. Homeopathy, for example, is not just without reason for working, it’s actually counter to reason.
I believe many of these methods mentioned here to be a fraud or at most a misplaced faith in something which doesn’t actually have any scientific reason behind it. Homeopathy, for example, is not just without reason for working, it’s actually counter to reason.